COMPREHENSIVE HEALTHCARE PROGRAM
EXAMINATION
EXAMINATION NETWORK INTRODUCTION
INTERNATIONAL COLLABORATION CENTER
WIH Global Healthcare Center
Health Screening & Imaging
International
Collaboration Center
Leading University Medical Center
WIH Global Healthcare Center
Health Screening & Imaging
International
Collaboration Center
Leading University Medical Center
o New York
o California
o Massachusetts
o Minnesota
o Ohio
o USA
Boston
New York
Los Angeles
Las Vegas
Miami
Hawaii
o Europe
Switzerland
o Africa
South Africa
o Asia / Pacific
Thailand: Phuket, Koh Samui
Indonesia: Bali
Philippines: Cebu
United Arab Emirates: Dubai
Australia: Sydney
o South-America
Brazil
Total 21 locations planned
(2024~)

o New York
o California
o Massachusetts
o Minnesota
o Ohio
The planned Location for WiH Global Healthcare Center
( VVIP & VIP )
for VVIP

USA : New York, Miami, LA, Las Vegas, Hawaii
Europe : Swiss
Africa : South Africa
Asia / Pacific : Thailand(Phuket, Koh Samui), Indonesia(Bali), Philippines(Cebu, Palawan), Australia(Sydney)
South America : Brazil
for VIP

USA : New York, Miami, LA, Las Vegas, Hawaii
Europe : Swiss
Africa : South Africa
Europe : Swiss
Asia / Pacific : Thailand(Phuket, Koh Samui), Indonesia(Bali), Philippines(Cebu, Palawan), Australia(Sydney)
South America : Brazil
USA
Europe
Africa
Asia / Pacific
South America
New York, Miami, LA, Las Vegas, Hawaii
Swiss
South Africa
Thailand(Phuket, Koh Samui), Indonesia(Bali)
Philippines(Cebu, Palawan), Australia(Sydney)
Brazil
USA
Europe
Africa
Asia / Pacific
South America
New York, Miami, LA, Las Vegas, Hawaii
Swiss
South Africa
Thailand(Phuket, Koh Samui), Indonesia(Bali)
Philippines(Cebu, Palawan), Australia(Sydney)
Brazil
for Middle Class

Asia / Pacific : Thailand(Phuket, Koh Samui, Chiang MAi), Indonesia(Bali), Philippines(Cebu), Vietnam(Da Nang)
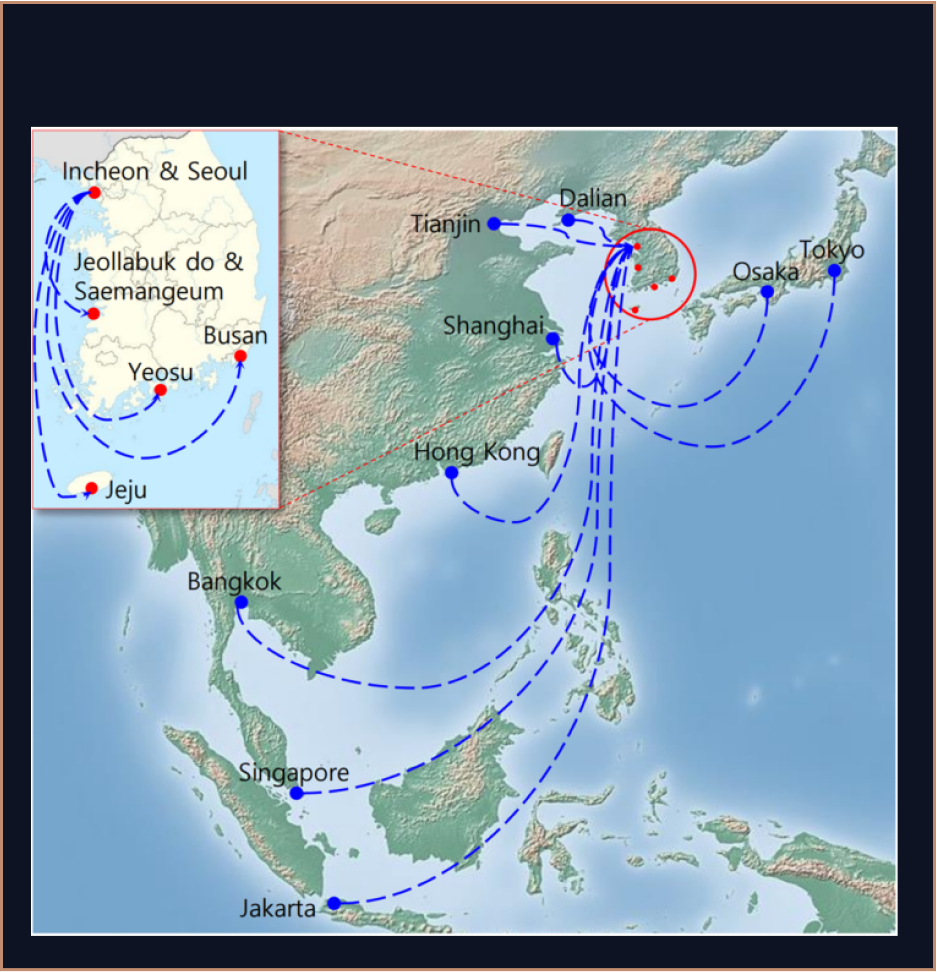
Asia-Region-Medical-Tour
EXAMINATION PROGRAM
HEALTH EXAMINATION PROGRAM
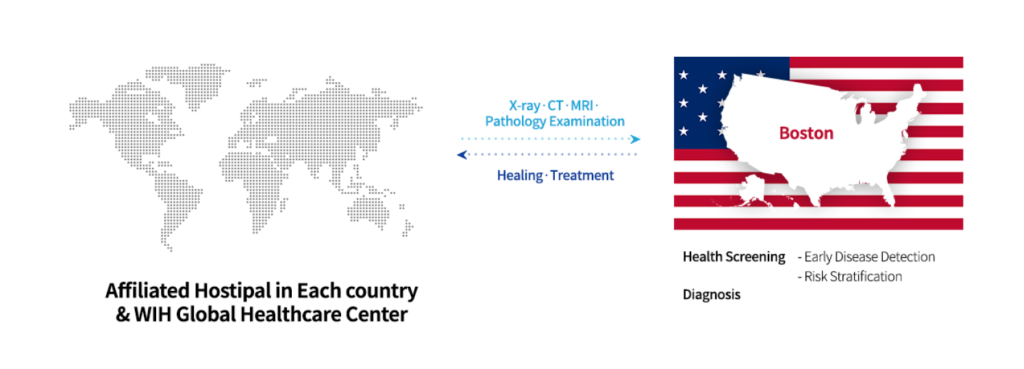
Program Overview
The examination data(each Center & Hospital) is transmitted to Harvard, where is read and diagnosed.
Patients in need of treatment will be transferred to the hospital, and customers in need of healing service (WiH Examination Package)
Program Type

Comprehensive
Medical Examination

Disease-specific
Special Examination
cardiology, neurology and
cancer clinical specialties
Special Examination
for Brain Disease
Using 7T MRI
Program Details
Examination
Field
Screening by special disease (brain disease / breast cancer, pancreatic cancer and various cancers / cardiovascular disease, etc.)
General screening
Health Examination Center
AI special examination system of Harvard MGH / MIT / partners hospital
The best medical Staff at famous American Univ. hospitals
Medi-Town in each Country
Reservation Procedure
NFT Purchase (Electronic Reservation Card): Sold on a first-come, first-served basis due to a limited number of examinations
Payment Method
WIHD Token
Where to buy WIHD Token
openwih.com
Special Disease (Cancer) Screening
PET-MRI
DNA Test
Transportation
Private Jet : Examinations at Global Center
Air Charter Service : Corporate group Examinations
Special examination for Brain Disease
7T MRI
WIH World Inc. @ USA
Leading Medical Centers
- New York
- California
- Massachusetts
- Minnesota
- Ohio

· Advanced medical service for VVIP, VIP customers through Global Center
· Advanced non-face-to-face treatment, diagnostic service
· Global Stable Cryptocurrency (WIH Pay : Payment method)
· Using 7T MRI (High-Tech Brain Imaging Diagnosis)
EXAMINATION PROGRAM
BRAIN HEALTH PROGRAM
Overview
Modern health and wellness approaches preserve the body. Without a healthy brain however, a healthy body alone will not provide the quality of life and mind that we all want as we age. TS Imaging Laboratories provides bespoke brain health screening tools to empower the individual to delay cognitive decline that occurs with age.
Using the world’s most advanced brain imaging technology, TS Imaging Laboratories creates a digital twin of your brain to monitor for minute changes that may be indicative of cognitive decline.
During your first visit, TS Imaging Laboratories performs a proprietary brain scan that will establish a baseline brain health report. With this report in mind, recommendations for potential activities that will enhance brain health will be provided.
Over time, through a series of regular visits, TS Imaging Laboratories monitors for changes in the digital twin of the brain to alert you of potential negative changes that will enable you to seek specific therapeutic intervention to halt the impact of those negative changes.
TS Imaging Laboratories is a combination of a luxury hotel spa and a health clinic. Each customer will have private access to the facility and confidentiality will be maintained to the utmost extent.
We understand that those that are willing to invest in their brain health would prefer their visit be part exam and part relaxation.
Baseline Brain Scan
An individual brain health report
Monitoring Brain Scan
Description of changes to the individual’s brain between scanning sessions
Health Intervention Recommendations
Network of health and wellness experts that utilize different approaches to improving brain health (massage, acupuncture and transcranial magnetic stimulation.)
Special Imaging Equipment
We have just recently entered a new brain imaging landscape based on the availability 7- Tesla magnetic resonance imaging (MRI) technology. ‘MRI’ is a brain imaging procedure that uses a highly powerful magnet to obtain detailed images of the body.
Although now commonly associated with electric cars, in MRI, ‘Tesla’ refers to the strength of the magnetic force used for imaging. The greater the strength of the magnet, the more powerful the imaging is. A typical scanner used for hospital imaging is either 1.5-Tesla, or 3-Tesla.
The resulting 7-Tesla scanner is over twice as powerful as all other common human imagers. This additional power allows measurement of brain properties at much greater detail.
In parallel, modern developments in computing hardware, software and statistical algorithms permit high computational processing of the information in the brain images providing extremely detailed assessment of the images that can be used in clinical as well as pre-clinical brain health applications including generation of the Brain Health Report.
Brain Health Report
The brain health report provides the ultimate result of the full brain mapping procedure.
This evaluation includes two sections.
FIRST SECTION

The first section is the clinical decision support report, providing information about any abnormalities detected that may require additional medical attention.
The accompanying figure provides clinical information, including medical referral type if applicable, a ‘predicted brain age’ (individual brain age compared to real age), a detailed color-coded image of any regions of the brain that show abnormalities, specific information about regions of the brain that are particularly vulnerable to degeneration from Alzheimer’s and cerebrovascular disease, and a comprehensive interpretation of the imaging information.
SECOND SECTION

The second section is targeted to the individual, not to the clinician or scientist. This section provides a description of the individual’s brain measures in layman’s terms.
This may include basic information about abnormalities, as described in the clinical section.
However, this section will be more directed towards education of the individual about their own brain.
Premium Brain Health Report
With a special super-powerful magnetic resonance imaging (‘MRI’) scanner and cutting- edge artificial intelligence-based image processing algorithms, we can now quantify the strength of multiple aspects of brain anatomy and physiology including measurement of the cerebral gray matter, the white matter brain connections, and brain functional activity.
These quantitative neural features are entered into analytical systems to derive novel personalized insights.
Technical Innovations
To generate a high-quality brain health report, Acuity Laboratories relies on the combination of two key technological innovations.
7T MRI Scanners
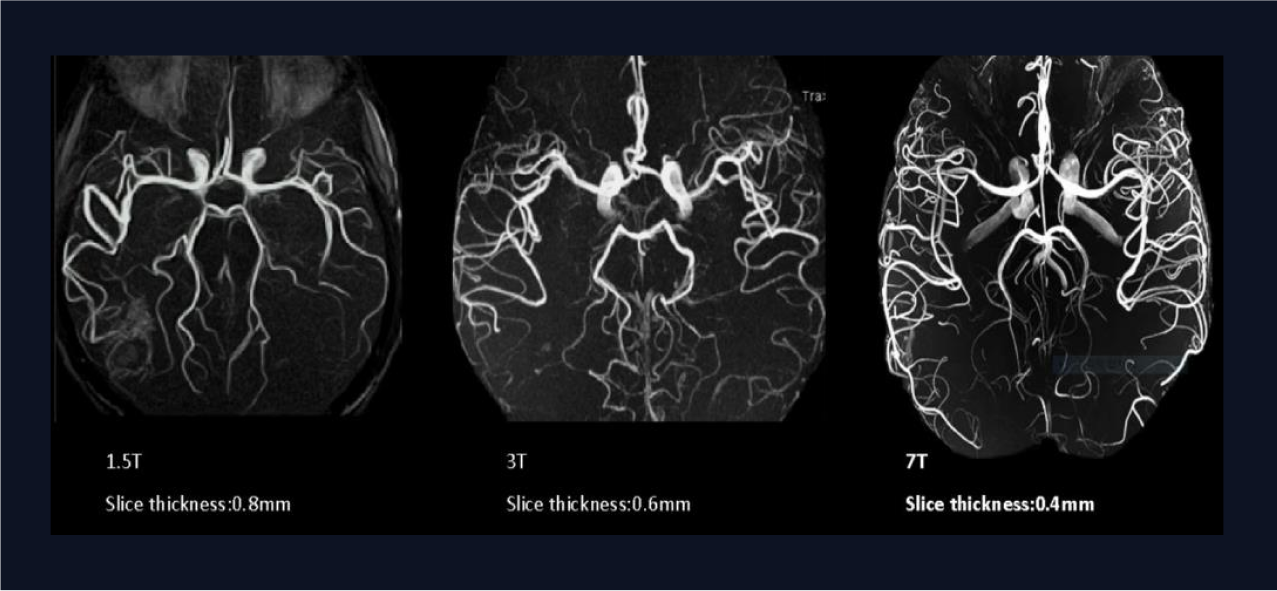
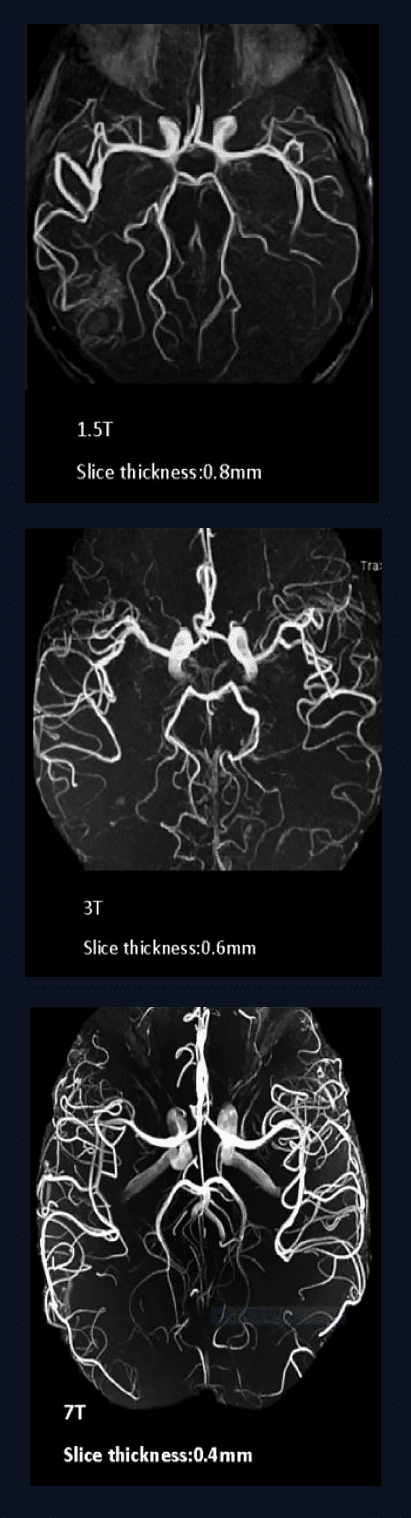
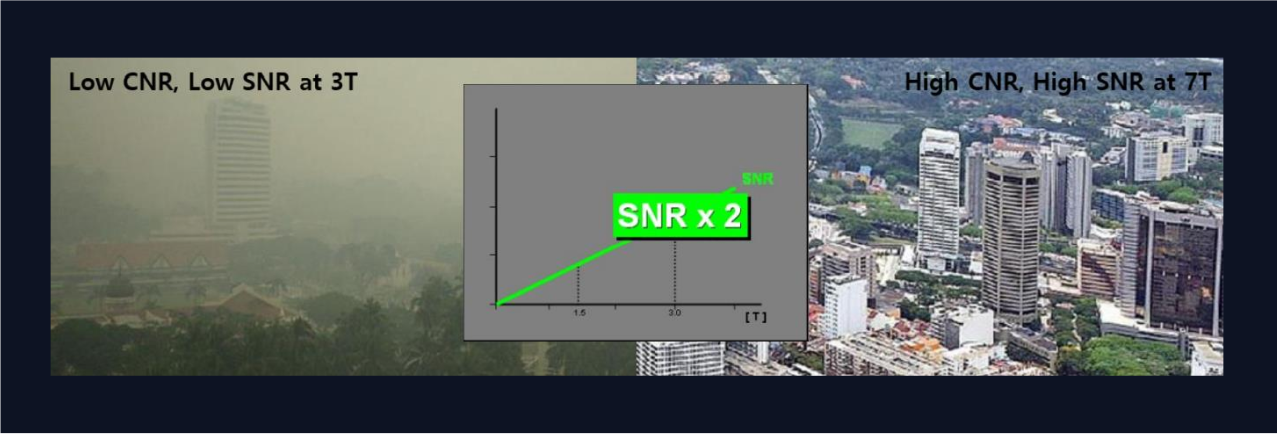
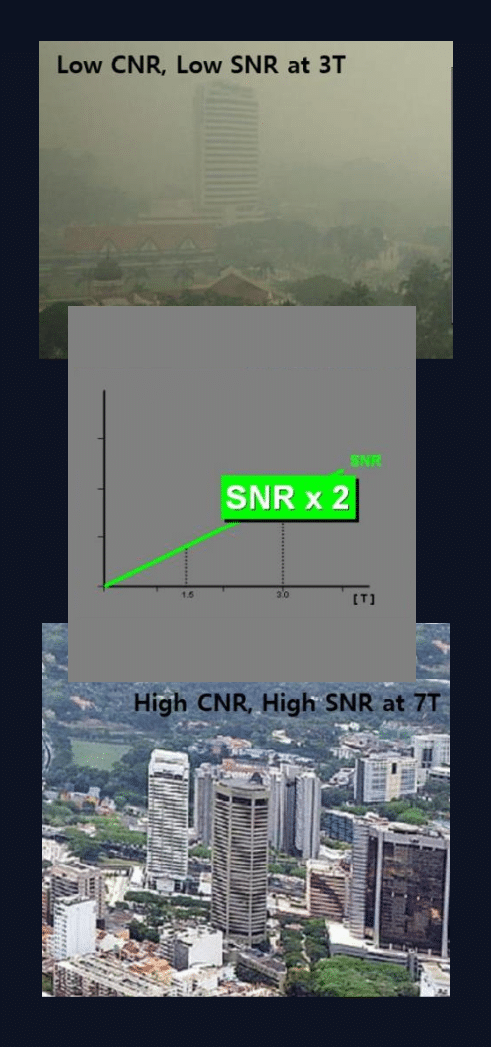
High-resolution MR images can depict rich details of brain anatomical structures and show subtle changes in longitudinal data. 7T MRI scanners can acquire MR images with higher resolution and better tissue contrast than the routine 3T MRI scanners.
When it comes to improving patient outcomes by answering the most challenging clinical questions, enabling deeper insights can make a difference. With double the SNR of 3T, imaging at 7T offers potential higher resolution in both anatomical imaging.
7T MRI can perform precise diagnosis and treatment with 100 times the superior resolution compared to the existing 1.5T or 3T MRI.
It was developed at Harvard and MIT and has been used in diagnostic and therapeutic research for the past 23 years.
All of our Healthcare Centers will provide precision imaging with 7T MRI (including PET) and diagnostics and medical services from renowned US university hospitals.
Resolution Comparison
EXAMINATION PETMRI SCREEMING
PET/MRI – A one-stop-shop
application for early
detection of common cancers
Introduction
Positron emission tomography (PET)/Magnetic resonance imaging (MRI) is an emerging imaging modality that combines the exquisite soft tissue contrast resolution of MRI and the picomolar sensitivity of PET1. By concomitantly acquiring metabolic and anatomical information, PET/MRI provides unparalleled co-registration of images, especially when combined with state-of-the-art motion correction techniques, and can leverage the full potentialities of MRI and PET2,3. PET/MRI, compared to PET/computed tomography (CT), cuts the radiation exposure by 30-60%4.
PET/MRI may serve as a one-stop-shop oncologic whole-body screening tool. Carefully matching tumor biology, acquisition protocols, and radiopharmaceuticals, PET/MRI represents the most advanced and best non-invasive diagnostic imaging technology.
Despite the huge number of possible cancers’ histology, PET/MRI protocols can be streamlined to just a few, based on common tumor metabolic pathways and patterns of spread. The most relevant and shared features among tumors are increased glycolytic metabolism, which is explored using 2-Deoxy-2-[18F]fluoroglucose ([18F]FDG), large extracellular tumor matrix, which exceeds the epithelial burden, and can be assessed through fibroblast activation protein inhibitor (FAPI) probes, and overexpression of some specific transmembrane receptors, which can be evaluated for example trough prostate-specific membrane antigen ligands (PSMA) and DOTATATE. In addition, specific MRI sequences can detect several non-metabolically active tumors that would be otherwise invisible on PET/CT. Therefore, tailored PET/MRI protocols that leverage tumor metabolism (PET) and tissue composition (MRI) can be employed for whole-body tumor evaluation.
The main class of tumors that may be explored by common radionuclide PET/MRI protocols are highlighted below. They encompass the vast majority of cancers. For example, prostate, lung, and colorectal cancers account for an estimated 43% of all cancers diagnosed in men in 2020; meanwhile breast, lung, and colorectal account for an estimated 50% of all new cancer diagnoses in women in 2020.
[18F]FDG-PET/MRI
Breast cancer
Invasive ductal carcinoma of the breast is the most common neoplasm worldwide, and its annual incidence continues to increase. On PET, this tumor is FDG avid5. [18F]FDG PET/MRI increases the diagnostic confidence6 and detects additional metastases, changing management in up to 39% of the cases. PET/MRI outperforms PET/CT7 reaching a sensitivity of 96% and a specificity of 99%8. PET/MRI can allow local staging, including the production of an accurate preoperative road map and whole-body evaluation.
Colorectal cancer
Colorectal cancer, the third most prevalent cancer, is usually FDG avid5. Whole-body [18F]FDG PET/MRI can be used for the detection of primary cancer, local and whole-body staging, outperforming standard imaging9. PET/MRI improves T staging10, assessment of tumor size, sphincteric infiltration11, N and M staging12–14 and may change patient management in 19%15 of the cases. Dedicated contrast enhanced PET/MRI protocols also allow the detection and staging of lobular cancer, which, being FDG negative, cannot be evaluated by PET/CT.
Lymphomas
Hematological malignancies account for 10% of cancers and up 5% of all new cases in 20225. [18F]FDG PET/MRI is equivalent to [18F]FDG PET/CT for FDG avid histotypes4,16–20, and through DWI can also be used to assess for non-FDG-avid lymphomas that might be missed on PET/CT 19.
Multiple myeloma
Multiple myeloma accounts for 2% of the expected new cancer cases in 20225. It primarily affects the bone marrow and causes lytic bone lesions. Low-dose CT enables adequate osseous evaluation if there is already an established diagnosis but is limited in the case of low tumor burden21–23. PET/MRI, instead, has higher sensitivity, is much less affected by tumor burden, and is not hampered by the degree of osetolysis24,25.
Lung
Lung tumors are highly lethal and responsible for 1 in 5 cancer-related deaths in 20225. In the context of non-small cell lung cancer (NSCLC), PET/MRI shows comparable results to PET/CT for initial staging26 and resectability determination27 (specificity 92%, sensitivity 97%, AUC 0.95 in the determination of resectability28). PET/MRI exceeds PET/CT and other standard-of-care imaging modalities in the evaluation of the brain, osseous, adrenals, and hepatic metastases.
PSMA PET/MRI
Prostate cancer
Prostate cancer, the most common cancer in males (27% of the newly diagnosed cancers), is PSMA-avid in about 90% of the cases, depending on tumor grade and histology29. [68Ga]Ga-PSMA PET/MRI is superior to PET alone and multiparametric MRI alone for prostate cancer localization (AUROCs of 0.88, 0.83, and 0.73, respectively)30, detection of extracapsular extension (69% vs. 46% )31, nodal staging and distant metastasis evaluation32–34. Overall, PSMA PET/MRI outperforms PSMA PET/CT also in the setting of biochemical recurrence, with a sensitivity of 99%35.
Renal Cancer
Renal tumors account for 4% of the new cancer diagnoses in the United States in 20225. A combination of dedicated MRI sequences, especially post-gadolinium acquisitions, DWI, STIR, and PSMA uptake can help detect primary renal neoplasms and whole-body metastases36–38
FAPI PET/MRI
Breast cancer
FAPI PET/MRI has been investigated in breast cancer. In one retrospective study, all 19 patients demonstrated [68Ga]Ga-FAPI uptake in the primary tumor, including patients with lobular carcinoma39. FAPI PET/MRI is expected to achieve extremely high sensitivity and specificity (close to 100%) and to outperform [18F]FDG imaging.
Colorectal cancer
[68Ga]Ga is superior to [18F]FDG in the detection of primary and metastatic lesions. FAPI also presents higher uptake in most lesions40. It has already been shown that [68Ga]Ga-FAPI leads to upstaging, when compared to [18F]FDG, in 21% of the cases.
Gastric cancer
Gastric cancer, the 5th most common cancer worldwide41. PET/MRI with [68Ga]Ga-FAPI has higher sensitivity than FDG imaging42 in primary tumor and distant metastasis detection43. [68Ga]Ga-FAPI also presents higher tumor-to-background ratio than [18F]FDG in gastric cancer. In signet ring cell adenocarcinoma specifically, the superiority of [68Ga]Ga-FAPI is even greater due to the known poor FDG avidity of these tumors44.
Pancreatic cancer
Pancreatic cancer is a deadly disease whose incidence is rising in the United States45. It is the 7th leading cause of cancer-related death worldwide46. [68Ga]Ga-FAPI PET/MRI, coupling the already superior performance of MRI in detecting and characterizing pancreatic tumors with the excellent sensitivity of FAPI, is expected to play a huge role in initial staging of pancreatic cancers, differentiation from benign pancreatic diseases, as well as accurate staging in more advanced disease47.
Cholangiocarcinoma
[68Ga]Ga-FAPI PET/MRI outperforms [18F]FDG PET/CT for detecting cholangiocarcinoma and extrahepatic metastases, especially in the peritoneum and bones48–50.
Central Nervous System
[68Ga]Ga-FAPI PET/MR is well suited to be the best ever imaging modality to assess brain metastases and might also play a crucial role in evaluating primary brain tumors as well as primary central nervous system lymphomas51–54.
Lung cancer
In lung adenocarcinoma, [18F]F-FAPI had comparable primary tumor detection rates to [18F]FDG, but showed higher tumor-to-background ratio and additional distant lesion detection55. [18F]FAPI also resulted in upstaging of 18% of the patients when compared to [18F]FDG.
References
1. Seifert R, Kersting D, Rischpler C, Opitz M, Kirchner J, Pabst KM, et al. Clinical use of PET/MR in oncology: An update. Semin Nucl Med. 2022 May;52(3):356–64.
2. Catalano OA, Umutlu L, Fuin N, Hibert ML, Scipioni M, Pedemonte S, et al. Comparison of the clinical performance of upper abdominal PET/DCE-MRI with and without concurrent respiratory motion correction (MoCo). Eur J Nucl Med Mol Imaging. 2018 Nov;45(12):2147–54.
3. Fuin N, Catalano OA, Scipioni M, Canjels LPW, Izquierdo-Garcia D, Pedemonte S, et al. Concurrent Respiratory Motion Correction of Abdominal PET and Dynamic Contrast-Enhanced-MRI Using a Compressed Sensing Approach. J Nucl Med. 2018 Sep;59(9):1474–9.
4. Atkinson W, Catana C, Abramson JS, Arabasz G, McDermott S, Catalano O, et al. Hybrid FDG-PET/MR compared to FDG-PET/CT in adult lymphoma patients. Abdom Radiol (NY). 2016 Jul;41(7):1338–48.
5. Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2022. CA Cancer J Clin. 2022 Jan;72(1):7–33.
6. Taneja S, Jena A, Goel R, Sarin R, Kaul S. Simultaneous whole-body 18F-FDG PET-MRI in primary staging of breast cancer: a pilot study. Eur J Radiol. 2014 Dec;83(12):2231–9.
7. Sawicki LM, Grueneisen J, Schaarschmidt BM, Buchbender C, Nagarajah J, Umutlu L, et al. Evaluation of 18 F-FDG PET/MRI, 18 F-FDG PET/CT, MRI, and CT in whole-body staging of recurrent breast cancer. Eur J Radiol. 2016 Feb;85(2):459–65.
8. Catalano OA, Nicolai E, Rosen BR, Luongo A, Catalano M, Iannace C, et al. Comparison of CE-FDG-PET/CT with CE-FDG-PET/MR in the evaluation of osseous metastases in breast cancer patients. Br J Cancer. 2015 Apr 28;112(9):1452–60.
9. Kang B, Lee JM, Song YS, Woo S, Hur BY, Jeon JH, et al. Added Value of Integrated Whole-Body PET/MRI for Evaluation of Colorectal Cancer: Comparison With Contrast-Enhanced MDCT. AJR Am J Roentgenol. 2016 Jan;206(1):W10-20.
10. Paspulati RM, Partovi S, Herrmann KA, Krishnamurthi S, Delaney CP, Nguyen NC. Comparison of hybrid FDG PET/MRI compared with PET/CT in colorectal cancer staging and restaging: a pilot study. Abdom Imaging. 2015 Aug;40(6):1415–25.
11. Catalano OA, Lee SI, Parente C, Cauley C, Furtado FS, Striar R, et al. Improving staging of rectal cancer in the pelvis: the role of PET/MRI. Eur J Nucl Med Mol Imaging. 2021 Apr;48(4):1235–45.
12. Lee DH, Lee JM, Hur BY, Joo I, Yi NJ, Suh KS, et al. Colorectal Cancer Liver Metastases: Diagnostic Performance and Prognostic Value of PET/MR Imaging. Radiology. 2016 Sep;280(3):782–92.
13. Yoon JH, Lee JM, Chang W, Kang HJ, Bandos A, Lim HJ, et al. Initial M Staging of Rectal Cancer: FDG PET/MRI with a Hepatocyte-specific Contrast Agent versus Contrast-enhanced CT. Radiology. 2020 Feb;294(2):310–9.
14. Zhang C, O’Shea A, Parente CA, Amorim BJ, Caravan P, Ferrone CR, et al. Evaluation of the Diagnostic Performance of Positron Emission Tomography/Magnetic Resonance for the Diagnosis of Liver Metastases. Invest Radiol [Internet]. 2021 Mar 25; Available from: http://dx.doi.org/10.1097/RLI.0000000000000782
15. Furtado FS, Suarez-Weiss KE, Vangel M, Clark JW, Cusack JC, Hong T, et al. Clinical impact of PET/MRI in oligometastatic colorectal cancer. Br J Cancer [Internet]. 2021 Jul 19; Available from: http://dx.doi.org/10.1038/s41416-021-01494-8
16. Mayerhoefer ME, Archibald SJ, Messiou C, Staudenherz A, Berzaczy D, Schöder H. MRI and PET/MRI in hematologic malignancies. J Magn Reson Imaging. 2020 May;51(5):1325–35.
17. Afaq A, Fraioli F, Sidhu H, Wan S, Punwani S, Chen SH, et al. Comparison of PET/MRI With PET/CT in the Evaluation of Disease Status in Lymphoma. Clin Nucl Med. 2017 Jan;42(1):e1–7.
18. Herrmann K, Queiroz M, Huellner MW, de Galiza Barbosa F, Buck A, Schaefer N, et al. Diagnostic performance of FDG-PET/MRI and WB-DW-MRI in the evaluation of lymphoma: a prospective comparison to standard FDG-PET/CT. BMC Cancer. 2015 Dec 23;15:1002.
19. Giraudo C, Raderer M, Karanikas G, Weber M, Kiesewetter B, Dolak W, et al. 18F-fluorodeoxyglucose positron emission tomography/magnetic resonance in lymphoma: Comparison with 18F-fluorodeoxyglucose positron emission tomography/computed tomography and with the addition of magnetic resonance diffusion-weighted imaging. Invest Radiol. 2016 Mar;51(3):163–9.
20. Guo R, Xu P, Cheng S, Lin M, Zhong H, Li W, et al. Comparison of nasopharyngeal MR, 18 F-FDG PET/CT, and 18 F-FDG PET/MR for local detection of natural killer/T-cell lymphoma, nasal type. Front Oncol. 2020 Oct 14;10:576409.
21. Hillengass J, Usmani S, Rajkumar SV, Durie BGM, Mateos MV, Lonial S, et al. International myeloma working group consensus recommendations on imaging in monoclonal plasma cell disorders. Lancet Oncol. 2019 Jun;20(6):e302–12.
22. Moulopoulos LA, Koutoulidis V, Hillengass J, Zamagni E, Aquerreta JD, Roche CL, et al. Recommendations for acquisition, interpretation and reporting of whole body low dose CT in patients with multiple myeloma and other plasma cell disorders: a report of the IMWG Bone Working Group [Internet]. Vol. 8, Blood Cancer Journal. 2018. Available from: http://dx.doi.org/10.1038/s41408-018-0124-1
23. Lambert L, Ourednicek P, Meckova Z, Gavelli G, Straub J, Spicka I. Whole-body low-dose computed tomography in multiple myeloma staging: Superior diagnostic performance in the detection of bone lesions, vertebral compression fractures, rib fractures and extraskeletal findings compared to radiography with similar radiation exposure. Oncol Lett. 2017 Apr;13(4):2490–4.
24. Cavo M, Terpos E, Nanni C, Moreau P, Lentzsch S, Zweegman S, et al. Role of 18F-FDG PET/CT in the diagnosis and management of multiple myeloma and other plasma cell disorders: a consensus statement by the International Myeloma Working Group. Lancet Oncol. 2017 Apr;18(4):e206–17.
25. Mulé S, Reizine E, Blanc-Durand P, Baranes L, Zerbib P, Burns R, et al. Whole-Body Functional MRI and PET/MRI in Multiple Myeloma. Cancers [Internet]. 2020 Oct 27;12(11). Available from: http://dx.doi.org/10.3390/cancers12113155
26. Lee SM, Goo JM, Park CM, Yoon SH, Paeng JC, Cheon GJ, et al. Preoperative staging of non-small cell lung cancer: prospective comparison of PET/MR and PET/CT. Eur Radiol. 2016 Nov;26(11):3850–7.
27. Messerli M, de Galiza Barbosa F, Marcon M, Muehlematter UJ, Stolzmann P, Warschkow R, et al. Value of PET/MRI for assessing tumor resectability in NSCLC-intra-individual comparison with PET/CT. Br J Radiol. 2018 Oct 11;20180379.
28. Fraioli F, Screaton NJ, Janes SM, Win T, Menezes L, Kayani I, et al. Non-small-cell lung cancer resectability: diagnostic value of PET/MR. Eur J Nucl Med Mol Imaging. 2015 Jan;42(1):49–55.
29. Ross JS, Sheehan CE, Fisher HAG, Kaufman RP Jr, Kaur P, Gray K, et al. Correlation of primary tumor prostate-specific membrane antigen expression with disease recurrence in prostate cancer. Clin Cancer Res. 2003 Dec 15;9(17):6357–62.
30. Eiber M, Weirich G, Holzapfel K, Souvatzoglou M, Haller B, Rauscher I, et al. Simultaneous 68Ga-PSMA HBED-CC PET/MRI improves the localization of primary prostate cancer. Eur Urol. 2016 Nov;70(5):829–36.
31. Muehlematter UJ, Burger IA, Becker AS, Schawkat K, Hötker AM, Reiner CS, et al. Diagnostic accuracy of multiparametric MRI versus 68Ga-PSMA-11 PET/MRI for extracapsular extension and seminal vesicle invasion in patients with prostate cancer. Radiology. 2019 Nov;293(2):350–8.
32. Donswijk ML, van Leeuwen PJ, Vegt E, Cheung Z, Heijmink SWTPJ, van der Poel HG, et al. Clinical impact of PSMA PET/CT in primary prostate cancer compared to conventional nodal and distant staging: a retrospective single center study. BMC Cancer. 2020 Aug 5;20(1):723.
33. Hofman MS, Lawrentschuk N, Francis RJ, Tang C, Vela I, Thomas P, et al. Prostate-specific membrane antigen PET-CT in patients with high-risk prostate cancer before curative-intent surgery or radiotherapy (proPSMA): a prospective, randomised, multicentre study. Lancet. 2020 Apr 11;395(10231):1208–16.
34. Zhao R, Li Y, Nie L, Qin K, Zhang H, Shi H. The meta-analysis of the effect of 68Ga-PSMA-PET/CT diagnosis of prostatic cancer compared with bone scan. Medicine (Baltimore). 2021 Apr 16;100(15):e25417.
35. Guberina N, Hetkamp P, Ruebben H, Fendler W, Grueneisen J, Suntharalingam S, et al. Whole-body integrated [68Ga]PSMA-11-PET/MR imaging in patients with recurrent prostate cancer: Comparison with whole-body PET/CT as the standard of reference. Mol Imaging Biol. 2020 Jun;22(3):788–96.
36. Rowe SP, Gorin MA, Hammers HJ, Som Javadi M, Hawasli H, Szabo Z, et al. Imaging of metastatic clear cell renal cell carcinoma with PSMA-targeted 18F-DCFPyL PET/CT. Ann Nucl Med. 2015 Dec;29(10):877–82.
37. Rhee H, Blazak J, Tham CM, Ng KL, Shepherd B, Lawson M, et al. Pilot study: use of gallium-68 PSMA PET for detection of metastatic lesions in patients with renal tumour. EJNMMI Res. 2016 Dec;6(1):76.
38. Meyer AR, Carducci MA, Denmeade SR, Markowski MC, Pomper MG, Pierorazio PM, et al. Improved identification of patients with oligometastatic clear cell renal cell carcinoma with PSMA-targeted 18F-DCFPyL PET/CT. Ann Nucl Med. 2019 Aug;33(8):617–23.
39. Backhaus P, Burg MC, Roll W, Büther F, Breyholz HJ, Weigel S, et al. Simultaneous FAPI PET/MRI targeting the fibroblast-activation protein for breast cancer. Radiology. 2022 Jan;302(1):39–47.
40. Pang Y, Zhao L, Luo Z, Hao B, Wu H, Lin Q, et al. Comparison of 68Ga-FAPI and 18F-FDG uptake in gastric, duodenal, and colorectal cancers. Radiology. 2021 Feb;298(2):393–402.
41. Rawla P, Barsouk A. Epidemiology of gastric cancer: global trends, risk factors and prevention. Prz Gastroenterol. 2019;14(1):26–38.
42. Jiang D, Chen X, You Z, Wang H, Zhang X, Li X, et al. Comparison of [68 Ga]Ga-FAPI-04 and [18F]-FDG for the detection of primary and metastatic lesions in patients with gastric cancer: a bicentric retrospective study. Eur J Nucl Med Mol Imaging. 2022 Jan;49(2):732–42.
43. Qin C, Shao F, Gai Y, Liu Q, Ruan W, Liu F, et al. 68Ga-DOTA-FAPI-04 PET/MR in the evaluation of gastric carcinomas: Comparison with 18F-FDG PET/CT. J Nucl Med. 2022 Jan;63(1):81–8.
44. Chen H, Pang Y, Li J, Kang F, Xu W, Meng T, et al. Comparison of [68Ga]Ga-FAPI and [18F]FDG uptake in patients with gastric signet-ring-cell carcinoma: a multicenter retrospective study. Eur Radiol [Internet]. 2022 Aug 17; Available from: http://dx.doi.org/10.1007/s00330-022-09084-9
45. Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020 Jan;70(1):7–30.
46. Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018 Nov;68(6):394–424.
47. Shou Y, Xue Q, Yuan J, Zhao J. 68Ga-FAPI-04 PET/MR is helpful in differential diagnosis of pancreatitis from pancreatic malignancy compared to 18F-FDG PET/CT: a case report. Eur J Hybrid Imaging. 2021 Jun 15;5(1):12.
48. Guo W, Pang Y, Yao L, Zhao L, Fan C, Ke J, et al. Imaging fibroblast activation protein in liver cancer: a single-center post hoc retrospective analysis to compare [68Ga]Ga-FAPI-04 PET/CT versus MRI and [18F]-FDG PET/CT. Eur J Nucl Med Mol Imaging. 2021 May;48(5):1604–17.
49. Siripongsatian D, Promteangtrong C, Kunawudhi A, Kiatkittikul P, Chotipanich C. 68Ga-FAPI-46 PET/MR detects recurrent cholangiocarcinoma and intraductal papillary mucinous neoplasm in a patient showing increasing CEA with negative 18F-FDG PET/CT and conventional CT. Nucl Med Mol Imaging (2010). 2021 Oct;55(5):257–60.
50. Siripongsatian D, Promteangtrong C, Kunawudhi A, Kiatkittikul P, Boonkawin N, Chinnanthachai C, et al. Comparisons of quantitative parameters of Ga-68-labelled fibroblast activating protein inhibitor (FAPI) PET/CT and [18F]F-FDG PET/CT in patients with liver malignancies. Mol Imaging Biol [Internet]. 2022 Apr 29; Available from: http://dx.doi.org/10.1007/s11307-022-01732-2
51. Yang J, Dong A, Zuo C. 68Ga-FAPI-04 PET/CT in solitary choroid plexus metastasis from renal cell carcinoma. Clin Nucl Med. 2022 Oct 1;47(10):885–7.
52. Fu W, Liu L, Liu H, Zhou Z, Chen Y. Increased FAPI uptake in brain metastasis from lung cancer on 68Ga-FAPI PET/CT. Clin Nucl Med. 2021 Jan;46(1):e1–2.
53. Hao B, Wu J, Pang Y, Sun L, Chen H. 68Ga-FAPI PET/CT in assessment of leptomeningeal metastases in a patient with lung adenocarcinoma. Clin Nucl Med. 2020 Oct;45(10):784–6.
54. Zhang Y, Cai J, Lin Z, Yao S, Miao W. Primary central nervous system lymphoma revealed by 68Ga-FAPI and 18F-FDG PET/CT. Clin Nucl Med. 2021 Aug;46(8):e421–3.
55. Li Y, Lin X, Li Y, Lv J, Hou P, Liu S, et al. Clinical utility of F-18 labeled fibroblast activation protein inhibitor (FAPI) for primary staging in lung adenocarcinoma: A prospective study. Mol Imaging Biol. 2022 Apr;24(2):309–20.
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
